Articular or hyaline cartilage is the tissue that covers bone surface of the knee which helps in smooth interaction between the two bones in knee joint. Articular cartilage often gets damaged because of direct blow to the knee, trauma, accidents or fall causing pain, swelling, stiffness, and limited movement of the knee. Furthermore, it has less capacity to repair by itself because of no direct blood supply to cartilage. Therefore, cartilage transplantation helps to replace the damaged cartilage and restore the normal functioning of the knee.
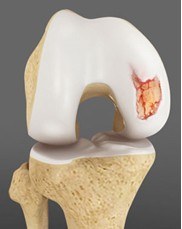
Cartilage Damage
Autologous cartilage implantation (ACI) is a technique of replacing the damaged cartilage by transplanting healthy cartilage. It is indicated in patients with full thickness large areas of articular cartilage damage. However, it is not recommended for patients having osteoarthritis.
Surgery is performed in two stages. In the first stage, the area of damage is identified to determine if ACI procedure is appropriate. The sample of a healthy cartilage cells is obtained from the damaged knee through arthroscopy. The cartilage cells are cultivated in the laboratory for 4 to 6 weeks.
In the second stage, incisions are made in knee and on the shin bone or tibia and the periosteal graft is harvested. The periosteal graft is taken from the periosteum tissue, which covers the tibia. This periosteal graft should match with the size of the damaged cartilage.
Next the periosteal patch is sutured over the damaged cartilage and cultured cartilage cells are injected below this patch. This patch holds the cultured cells in the defected area. Now the injected cartilage cells will begin to repair the damaged cartilage.
Complications of autologous cartilage implantation
- Periosteal hypertrophy – Scar tissue is formed around the periosteal patch. However, this scar tissue can be removed by arthroscopy.
- Improper integration of the newly implanted cartilage cells
- Infection of the knee
- Stiffness of the knee
Post-operative care
- Knee brace will be applied to restrict movement of the knee. At this stage, you will not be allowed to lift any heavy objects.
- Physiotherapy is recommended to regain the movement, reduce swelling, and helps the knee to bear the weight. Rehabilitation program includes various strengthening and stretching exercise which strengthens the quadriceps and hamstring muscles. It also helps to stimulate the growth of cartilage cells. With the consult of your doctor you will be able to return to sports.
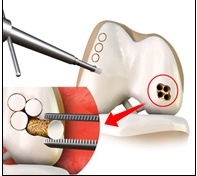
OATS Procedure
- Osteochondral Autograft Transplantation: Osteochondral autograft transplantation system (OATS) is a surgical procedure where plugs of cartilage are taken from the non-weight bearing areas of knee, from the same individual and transferred to the damaged areas of the joint. This method is used to treat smaller cartilage defects since the graft which is taken from the same individual will be limited.
- Osteochondral Allograft Transplantation: In this procedure, healthy cartilage tissue or a graft is taken from a donor from the bone bank and transplanted to the area of cartilage defect.
Following cartilage replacement your doctor may recommend physical therapy to help restore mobility and to impart the strength to the affected joint.